One in every nine patients who go into hospital in Australia suffers a complication: when something preventable goes wrong with their care. They might develop an infection from a hygiene breach, for instance, or be given the wrong dose or type of drug.
Or the complication might be less direct, such as becoming malnourished because you haven’t been monitored well enough, or developing a pressure sore because you’ve spent too long in the same position in your hospital bed.
A new Grattan Institute report, All complications should count: Using our data to make hospitals safer, reveals the risk of a complication varies markedly between hospitals. It argues that patients need to know about these risks, and hospitals need to have this information to help them reduce risks for patients.
Australian hospitals collect a lot of information about the patients they treat. This information is used to work out how much each hospital is paid for the work they do. But it should also be a powerful tool for improving safety of care.
Rate of complications
Our report shows that the rate of complications for people admitted for a same-day treatment is very low, around 3%. But an astounding one in four patients who have an overnight stay endures a complication.
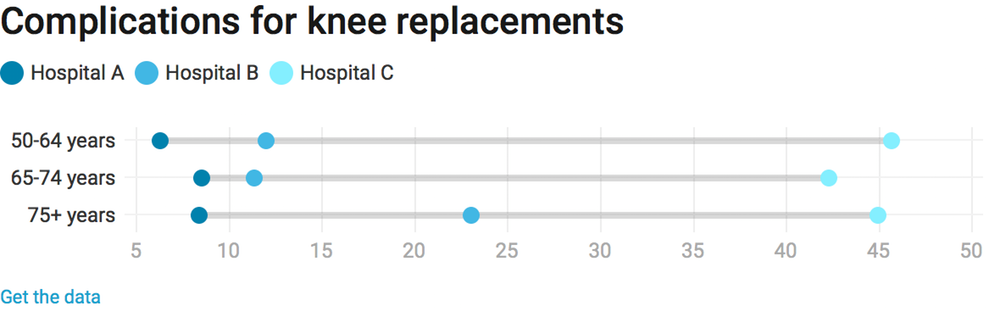
The rate of complications varies markedly between hospitals. We have data on every complication and every hospital, although the hospitals are de-identified. The potential value of this data is illustrated by the graph below, which looks at just one procedure – knee replacements – at three hospitals.
It shows Hospital A is a uniformly good hospital to go to for a knee replacement, and Hospital C is uniformly bad. At Hospital B, patients over 75 face twice the excess risk of a complication than patients between the ages of 50 and 74.
This isn’t all simply luck of the draw. Hospital A is obviously doing things better. Hospitals B and C may be lacking specialist geriatric support for elderly patients. The other hospitals should learn from Hospital A about how to lift their game.
Yet most Australian hospitals don’t receive this sort of detailed comparative information, so they cannot compare themselves to their peers and learn from the better performers.
Information needs to be shared
These huge variations in complication rates are important. More complications means more pain and discomfort for patients. Higher complication rates mean longer hospital stays, which in turn mean higher costs for the health system. Higher complication rates contribute to higher health insurance premiums, too.
Patients should have information about their chances of complications. They should know what their risk is, taking into account their age, gender and general state of health. They should also know what types of risks they face, from the rare but catastrophic to the less dramatic but more prevalent.
State governments and private health insurers have this information now. They should share it. They should publish information on complication rates at different hospitals, so that patients – and their referring general practitioners – can know what difference it makes, in terms of complications, going to one hospital compared to another.
This vital comparative complication rate information is generally not even provided to hospitals themselves. Although some states and some private health insurers have feedback programs – where they provide information adjusted for the mix of patients treated in the hospital – such programs are not universal, they are not comprehensive, and the data is often old.
This means hospitals are flying blind when designing safety improvement efforts. They don’t know how they are performing against their peers. They don’t know whether they are the best in class or the worst. They don’t know where they need to improve, or by how much they should improve. They don’t know how they measure up in terms of infection rates among their patients, or falls, or complications arising from procedures.
Worse, current government priorities encourage hospitals to focus on a subset of complications which only affect a fraction of patients and aren’t relevant to all specialties. This may lull hospitals into a false sense of security that they have no room to improve when in fact their overall performance – looking at all complications – may be very poor indeed.
How to reduce complications
Until all hospitals have all relevant information on their comparative complication rates, identifying where to start their improvement efforts is impossible. Our report recommends four simple solutions:
- all states and territories establish goals for reducing the overall rate of complications in public and private hospitals
- all states and territories give hospitals and clinicians the ability to interrogate the state hospitals data (without individual patients being able to be identified), so they can see how their performance measures up against the best-performing hospitals and clinicians. All hospitals develop strategies to identify opportunities to improve
- all states and territories publish reports on excess complications, by specialty and institution (including private hospitals)
- major private health insurers provide their members with comparative information on complication rates.
All these proposals could be implemented tomorrow. For the sake of Australian taxpayers and hospital patients, they should be.
Stephen Duckett is the Director, Health Program, Grattan Institute. Christine Jorm is an Associate professor, University of Sydney. Greg Moran is an Associate, Grattan Institute
This article first appeared in The Conversation on 5 February 2018
Stephen Duckett, an economist, is an Honorary Enterprise Professor in General Practice and in Population and Global Health at the University of Melbourne, Chair of the Board of Eastern Melbourne Primary Health Network, and a member of the Strengthening Medicare task force.

Comments
2 responses to “STEPHEN DUCKETT, CHRISTINE JORM AND GREG MORAN. Hospitals are risky places – but some are better than others”
Much may be done simply by doing what IS done – properly.
I have seen cleaning-staff at a famous teaching hospital flush the ‘loo in place of taking a brush, cleaning-agent and wipe to it; and I have handled trays tacky to the touch -underside- because the cleaning-cloths have just NOT been applied between uses – several/many uses. These 2 small examples, alone, could, under poor conditions, enable growth/spread of infection which, otherwise, need not exist at all.
Like so much other tax-funded obligations – these ‘services’ had been removed from hospital duties and ‘outsourced’ to ‘private’ suppliers.
“Prevention is better than cure.”
A number of my own, family members’ and friends’ experiences have led me to advise everyone with whom I discuss hospital admission (even to the most prestigious hospitals in Sydney) as follows:
Make sure that a family member or close friend is with you continuously from the moment of your admission, whether arranged in advance or through Accident & Emergency, until you go to the operating theatre, and then after you leave Recovery until you go home.
The nursing shortage is chronic. Nurses do not have the time to check that you drink enough, that you actually eat your meals, that you have those ordered blood tests, x-rays etc, that you get the correct medications, (especially when the hospital insists that you use new packs of whichever generic brand they happen to stock – and which you do not recognise) and that the other specialists called in on your problem actually arrive.
“You need a guardian angel,” is my advice. You might need a roster of such ‘angels’.
No aspersions on the nurses – they do the best they can. Unfortunately, it is often not enough.